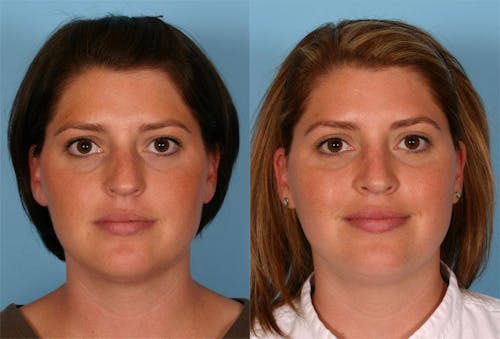
Surgeons at the Buckingham Center for Facial Plastic Surgery offer nasal obstruction solutions for patients in Austin, TX and the surrounding areas.
What Is Septoplasty?
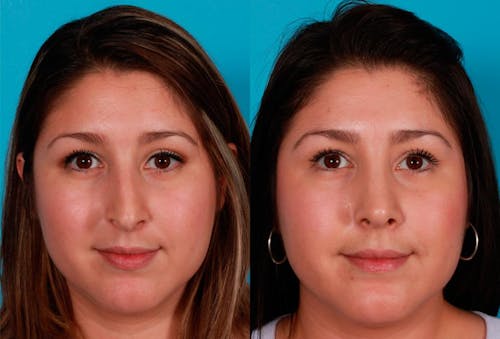
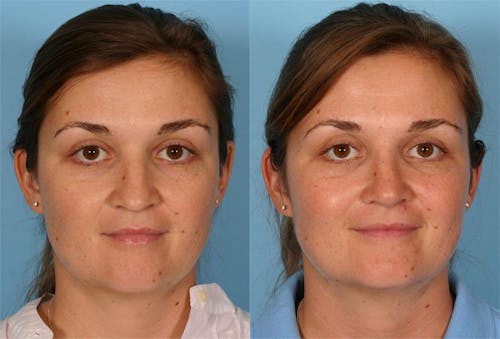
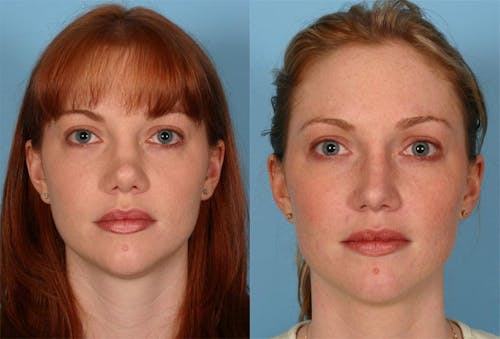
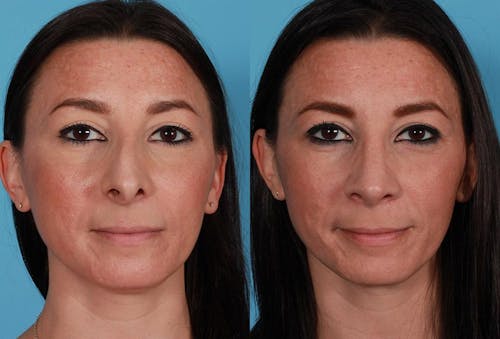
Functional nasal surgery can be performed to improve a patient’s ability to breathe through the nose, specifically by resolving anatomical problems leading to nasal obstruction. This may involve a septoplasty, turbinate reduction, nasal valve repair, or nasal bone correction. A septoplasty is a procedure that surgeons use to straighten the cartilaginous and bony septum of the nose. The septum is the structure that separates the left and right nostrils.
Internal and external nasal valve repair involves reinforcing the structural components of the nose. When a patient has already had a septoplasty, our surgeon typically uses cartilage grafts harvested from redundant portions of the patient’s nasal septum or ear to support the sidewalls of the nose and the nostrils. . During turbinate reduction, the surgeon removes excess tissue and bone from the inferior turbinates on the inside of the nose, which might be causing further narrowing of the nasal cavity. A nasal bone correction is a procedure where the collapsed or deviated nasal bones are re-structured to a more midline and symmetric position.